Uganda is still battling with high numbers of lymphatic filariasis (elephantiasis), schistosomiasis (Bilharzia), soil-transmitted helminths (intestinal worms), onchocerciasis (river blindness), trachoma, human African trypanosomiasis (sleeping sickness), visceral leishmaniasis (Kala-azar), plague, Buruli ulcer disease, rabies, tungiasis (jiggers), podoconiosis (non-filarial elephantiasis), echinococcosis, cysticercosis, brucellosis and leprosy. As a commnuity healthcare support organisation with hubs across the country, our role remains to engage sustainable recommendations and improve support to communities toparticipate in ending such illnesses by strengthening community healthcare strategies and deploying protective interventions.
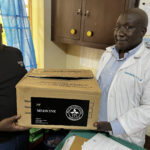
Our teams are on the ground to engage with VHTs, community leaders and community groups to participate in the preventive methods that will support the elimination of NTDs infections. Our consultants, following the 2019 MoH Consultations on NTDs in Uganda continue to move with RHU teams to train and prepare RHU Community groups and VHTs for the deployment of preventive measures (including prophylaxis) in communities where RHU Operates. Today the teams are in Eastern Uganda to continue efforts that address tungiasis among other illnesses and have engaged with community leaders in various parts of Eastern Uganda.
Coordination of NTD services is one of the challenges cited during the MoH NTDs consultation and one of the reasons why RHU integrated specific interventions for NTDs in our action plan and thus such community engagements. Our community structures have aided coordination of services to address operational capacity and services delivery. The Skilling of more of our community members at this level is challenged by resources to facilitate activities that promote prevention and access to healthcare services at community level. Our bid remains maintaining the available systems and find support to promote prevention and information flow.
162 community leaders and VHT group members have so far been engaged to forge ways on community integration, treatment dissemination and community alert systems to support early interventions. The activity will continue into 2022 and deployment of preventive and supportive strategies is expected to commence in december 2022 through out 2024 following WHO’s road map on NTDs 2021-2030.